ICU Medicine Is a Team Sport
By: Sue Stempek, PA-C, MS, FCCP
March 20, 2017
I am incredibly fortunate to work on a multidisciplinary team every day. The team includes respiratory therapists, nurses, nutritionists, attending physicians (APs), and advanced practice providers (APPs) (nurse practitioners [NPs] and physician assistants [PAs]).
Our APPs provide comprehensive care to critically ill patients. We evaluate patients independently in the emergency department, admit patients to the ICU, and perform procedures. We meet with families, facilitate transfers out of the ICU, respond to rapid response team calls, and evaluate critically ill patients outside the ICU and formulate treatment plans.
The involvement of APPs allows the attending physician the time to focus on physiologic complexity associated with tertiary care, to perform specialty procedures, and to review their own patients in the ICU. Once fully trained, we can extend provider coverage by delivering evidence-based critical care at the bedside.
Given the very short time spent in formal provider training programs by both NPs and PAs we recognized the need to expand the technical skill set of APPs delivering critical care at the bedside. Critical Skills for Critical Care (August 11-13) is a Live Learning course focused on expanding the procedural and diagnostic skill set of APPs.
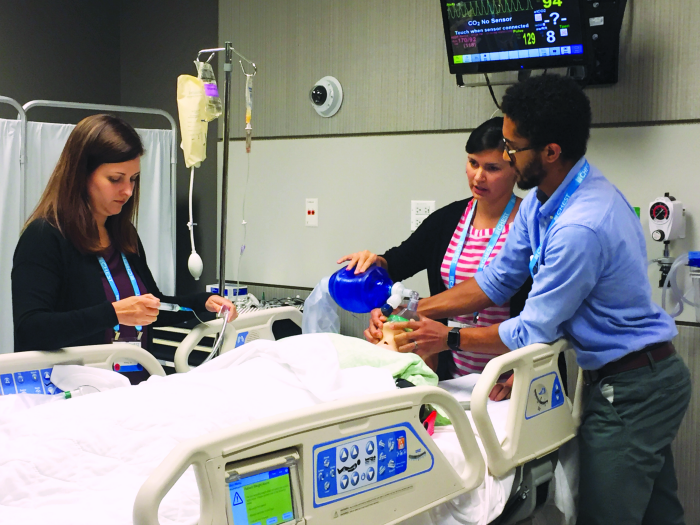
Evidence-based critical care medicine is not easy to teach; but based on nuances of individual sites, programs may want to focus clinical specifics on high-yield topics when training APPs. Throughout my career my interest in formal training of critical care APs has grown exponentially. No matter the training program of an NP or PA, it is certainly rare for them to have encountered many critical care procedures.
It is also uncommon for these new practitioners to have had adequate training in bedside diagnostics, such as basic critical care ultrasound. As leaders in APP critical care, it is our charge to provide this education to accelerate the ability of these providers to provide high-quality patient care to critically ill patients.
Throughout my career I have been fortunate to have been taught by many high-quality clinicians, notably many physicians who believe in a care delivery model that includes APPs. I believe the engagement of these colleagues in the process of educating myself and countless other APPs has played a critical role in elevating the ability of health-care systems in delivering high-quality, cost-effective, critical care services.
There is no question a large responsibility is incumbent on the APP to invest in his or her own ongoing education with didactic learning and simulation. The combination of physician colleague commitment as well as continued interaction with excellent educational opportunities will support the contribution of APPs to patient and family satisfaction as well as optimal outcomes.
Register for Critical Skills for Critical Care.

Sue Stempek, PA-C, MS, FCCP is the Director of Advanced Practice at Lahey Hospital and Medical Center in Burlington, MA where she also works in a clinical capacity in the ICU. She has been in practice as a pulmonary and critical care Physician Assistant for 12 years and has a special interest in high quality education for nurse practitioners and physician assistants in critical care specialties.