Patent Foramen Ovale: A Cause for Refractory Hypoxemia
By: Dr. Jacqueline Greer
February 8, 2019
Up to 25% of adults have a patent foramen ovale (PFO).1 Patients with chronic obstructive pulmonary disease and pulmonary hypertension are at significantly increased risk of having PFO relative to the general population.1 Pulmonary and critical care providers are often evaluating patients with hypoxemia and need to know when to consider assessment for PFO in their evaluation of refractory hypoxemia. We present a framework for assessing patients with PFO.
How is PFO diagnosed?
PFO should be considered in patients with refractory hypoxemia or platypnea-orthodeoxia syndrome (POS). There are invasive and noninvasive ways to identify a PFO. Gold standard tests include right heart catheterization with guidewire passage across the atrial septum and transesophageal echocardiogram (TEE) with agitated saline contrast. TEE allows for direct visualization of septal anatomy and can differentiate among PFO, atrial septal defect, and pulmonary shunt, but it can miss PFO in up to 10% of patients.2 The most common diagnostic test is transthoracic echocardiography (TTE) with agitated saline contrast. Appearance of “early” bubbles in the left heart (within three to five beats) indicates intracardiac shunting. Later appearance of bubbles suggests pulmonary arteriovenous shunting. Of note, transcranial doppler can identify shunt physiology but cannot distinguish between cardiac and pulmonary etiologies.2
What causes a PFO to open?
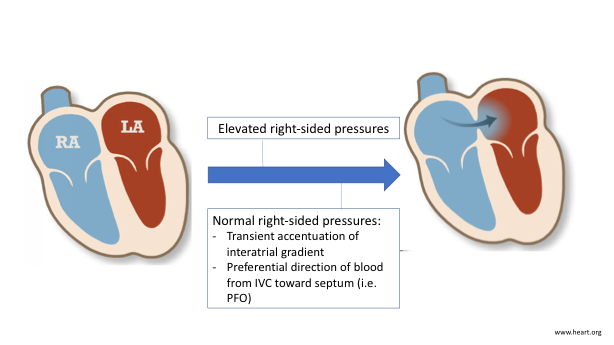
First, right-sided cardiac pressures must be determined. When elevated, as in pulmonary hypertension, a PFO can open as a “pop-off valve” with subsequent right-to-left shunting of blood.2 Although counterintuitive, right-to-left shunting can also occur with normal right-sided pressures due to transient accentuation of interatrial gradient or preferential direction of blood from the inferior vena cava (IVC) toward the PFO. The former can occur with physiologic, transient pressure changes such as early ventricular systole when there is a brief pressure reversal, normal respiratory cycle when venous return is augmented on inspiration and elevates atrial pressure (RAP) and decreases intrathoracic pressure, and release from Valsalva leading to a sudden increase in RAP.3 The latter mechanism can occur due to persistent Eustachian valve, ascending aortic aneurysm or root dilation, and post-pneumonectomy.4
When should PFO closure be considered?
PFO closure is considered in patients with cryptogenic stroke, divers with decompression illness, and those with refractory hypoxemia and/or POS. No guidelines exist for PFO closure leading to hypoxemia; however, case series and anecdotal evidence suggest dramatic symptomatic relief post-closure.5 Closure should be avoided in patients with high right-sided pressures as this can lead to clinical decline.2
Dr. Jacqueline Greer is an internal medicine specialist at Yale New Haven Health System.
References
- Layoun ME, Aboulhosn JA, Tobis JM. Potential role of patent foramen ovale in exacerbating hypoxemia in chronic pulmonary disease. Texas Heart Institute Journal. 2017;44(3):189-197.
- Mojadidi MK, Ruiz JC, Chertoff J, et al. Patent foramen ovale and hypoxemia. Cardiology in Review. 2019;27(1):34-40.
- Strunk BL, Cheitlin MD, Stulbarg MS, Schiller NB. Right-to-left interatrial shunting through a patent foramen ovale despite normal intracardiac pressures. American Journal of Cardiology. 1987;60(4):413-415.
- Godart F, Rey C, Prat A, et al. Atrial right-to-left shunting causing severe hypoxaemia despite normal right-sided pressures - Report of 11 consecutive cases corrected by percutaneous closure. European Heart Journal. 2000;21(6):483-489.
- Guerin P, Lambert V, Godart F, et al. Transcatheter closure of patent Foramen ovalle in patients with platypnea-orthodeoxia: Results of a multicentric French registry. Cardiovascular and Interventional Radiology. 2005;28(2):164-168.