Dual Physician Households During Training
By: Rachel Quaney, MD*
August 21, 2020
*With begrudging acceptance from Michael Haden, MD.
I recently searched haphazardly for some sex-based research articles from years past. One of the internet searches comically suggested one titled, “Why to not marry a female physician.” I laughed because the search engine algorithm needs some fine tuning, but also partly because there are certain days that I’m sure my husband agrees. In his defense, the eyeroll he offered when I mentioned this search warmed my cold, little heart.
Neither my husband nor I planned on finding a partner within medicine. In fact, my family lovingly likes to remind me of the days when I said I would never date a doctor. Fortunately, life often has its own plans, as third year of medical school brought dating a fellow student, then engagement, then a marriage in short succession.
We knew next to nothing about medical training, and we knew even less about marriage. But we did know that we wanted to figure this out together. And that is exactly what we have done so far.
Together we couples-matched to internal medicine, moved halfway across the country, and managed residency. We then couples-matched to fellowships—him in infectious diseases and me in pulmonary and critical care medicine—before moving again. More than 5 years into this marriage and now we find ourselves in the midst of a viral pandemic intimately involving our two specialties. What a ride.
Next up will be managing my hopeful match into sleep medicine while he begins his career as faculty. We now know a lot more about medical training and a little more about marriage. We have simultaneously navigated the highs and lows of both.
I don’t believe there is a singular answer to many things in life, and medical training in a dual-physician household is no different. But seeing as how we knew no one in our exact situation to readily contact for advice, the least we can do is share a few of the lessons we learned along the way.
Most of the lessons we did garner relate to flexibility, compromise, communication, and routines.
Like others pursuing the couples’ match, we realized the process can become convoluted when you’re combining two people’s interests. Unlike other careers, you don’t have the luxury of taking your time to explore a variety of locations and job opportunities. Instead, you have one opportunity to apply to programs and hope that you included the best ones for you both. There is no way to reference data from similar scenarios, because there is no corollary to Charting Outcomes in the Match for the couples’ match. However, there are general data that demonstrate a couples’ match rate of 95% or higher for the past 4 years,1 as members of the National Board of Medical Examiners do take couples’ matching into consideration.
But with both individuals depending on student loans and navigating nerve-wracking career prospects, this time can be stressful. Each person has poured themselves into getting to this point that defines their future career, but you must balance the interests of each individual—hence communication, compromise, and flexibility. Often this requires a very frank conversation about your strengths and weaknesses as individual applicants, then a comically convoluted process of adding and subtracting programs to your application list, considering geography, prestige, program characteristics, and other factors.
Some couples form their list based on large cities so they can list one city’s programs as a multitude of matches (Figure 1). Others start with program characteristics. We started our list based on geography, factoring in areas we wanted to live.
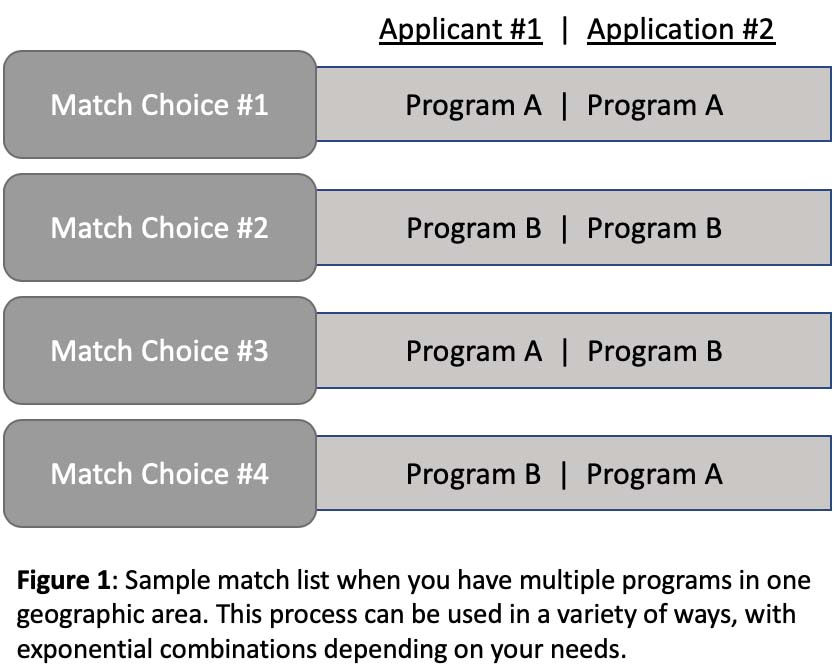
Regardless of which method selected, it makes sense to start your list with the most particular partner’s choices. Does one partner need a program with a particular subspecialty hospital certification for their career goals? Start there. Does one partner have health needs and need to be near their providers or near their family? Start there.
The interview season is challenging for all, and there is no advice that provides a panacea, so I won’t pretend that it does. However, I do know that my husband and I chose to take advantage of the fact that we were applying to the same specialty for residency. We politely asked for the same interview days, and the few locations that were not willing to accommodate this request were removed from our potential list of programs. Our opinion was this indicated their future unwillingness to work with our schedules during training. We then looked at interview trips as adventures, because we had very little money but a plethora of time. If the cheapest flight was at an inconvenient time, then we went with it. This led us to wandering around new cities and exploring whatever came our way. We will never again have time and experiences like that, so we chose to cherish it.
After match season and graduation, we moved halfway across the country to the next chapter, where we slept on the floor in our new home and anxiously awaited our first paychecks! Residency brings personal and marital challenges but also room for growth in both arenas. Although I wholly appreciate the ability to debrief medical dilemmas with my spouse and have a sounding board I explicitly trust, we did struggle to separate work from home.
He taught (forced?) me to log off from the electronic medical record system once at home, and we strove to reconnect as a couple. We instituted what we termed “flexible routines.” We could not guarantee when we would arrive home from work, but we craved a signal that work time was complete and family time should commence. Thus, we developed a routine for when the second person arrived home.
We would walk the dog and debrief about our days, and we discovered this physical signal that the workday was transitioning to family time gave us our nights back, regardless of how little time that was. He began to prepare coffee at night, so I had caffeine immediately upon waking, which is better for everyone involved, and also served as a symbol of affection on days we didn’t see each other. Friday nights became pizza nights. These flexible routines were never fancy but were ours and marked our time outside of the hospital walls.
This flexibility came in handy when it was time to apply for fellowship! The second round of interviews was wildly different than the first. We could afford reasonable travel arrangements but had a shortage of available time. Between clinical rotations, other educational responsibilities, and staggered interviews, we went months without quality time together.
We were burnt out and not bringing our best selves to the marriage, but we knew what to do: back to intentional time with one another and back to flexible routines. It’s not always pretty, but, step by step, we work back to the balanced marriage that reminds me why I am happy fate laughed in my face and brought this brilliant, stubborn man into my life. I enjoy figuring out this journey with him at my side.
Reference:
1. National Resident Matching Program. Results and Data: 2019 Main Residency Match®  . National Resident Matching Program; Washington, DC: 2019.
. National Resident Matching Program; Washington, DC: 2019.

Rachel Quaney, MD, is Chief Fellow in pulmonary and critical care medicine at The Ohio State University and currently pursuing a master’s degree in medical education. Her clinical interests include respiratory failure and mechanical ventilation, ranging from critical care to those served in sleep medicine. Her research interests are in medical education and center on feedback, assessments, and coaching. She is active in the medical education community, serving on the CHEST Trainee Work Group, the Association of Pulmonary and Critical Care Medicine Program Directors Fellows’ Working Group, the American Thoracic Society (ATS) Training Committee, and as Co-Chair of ATS Trainees Interested in Medical Education.